Introduction of Crystalline Penicillin and Benzylpenicillin
Crystalline Penicillin and Benzylpenicillin both belong to the penicillin class of antibiotics. Crystalline Penicillin, often referred to as penicillin G, is produced from natural sources and can take the form of powder or crystals. Its wide spectrum antimicrobial activity often treats severe infections.
Conversely, Benzylpenicillin V, commonly administered orally as oral treatment is often more stable and suitable for less severe infections. Each antibiotic differs in chemical structure, production methods, stability levels, medical applications, and patient needs.
So healthcare professionals must choose an appropriate penicillin depending on which infection needs they treat or patient needs they meet.
What is Crystalline Penicillin?
Crystalline Penicillin (also known as penicillin G) was the pioneer of the penicillin class when first discovered by Alexander Fleming in 1928. Characterized by its distinct chemical structure and production through Penicillium molds, Crystalline Penicillin provides broad antimicrobial activity against multiple bacterial infections and should preferably be given by injection rather than orally.
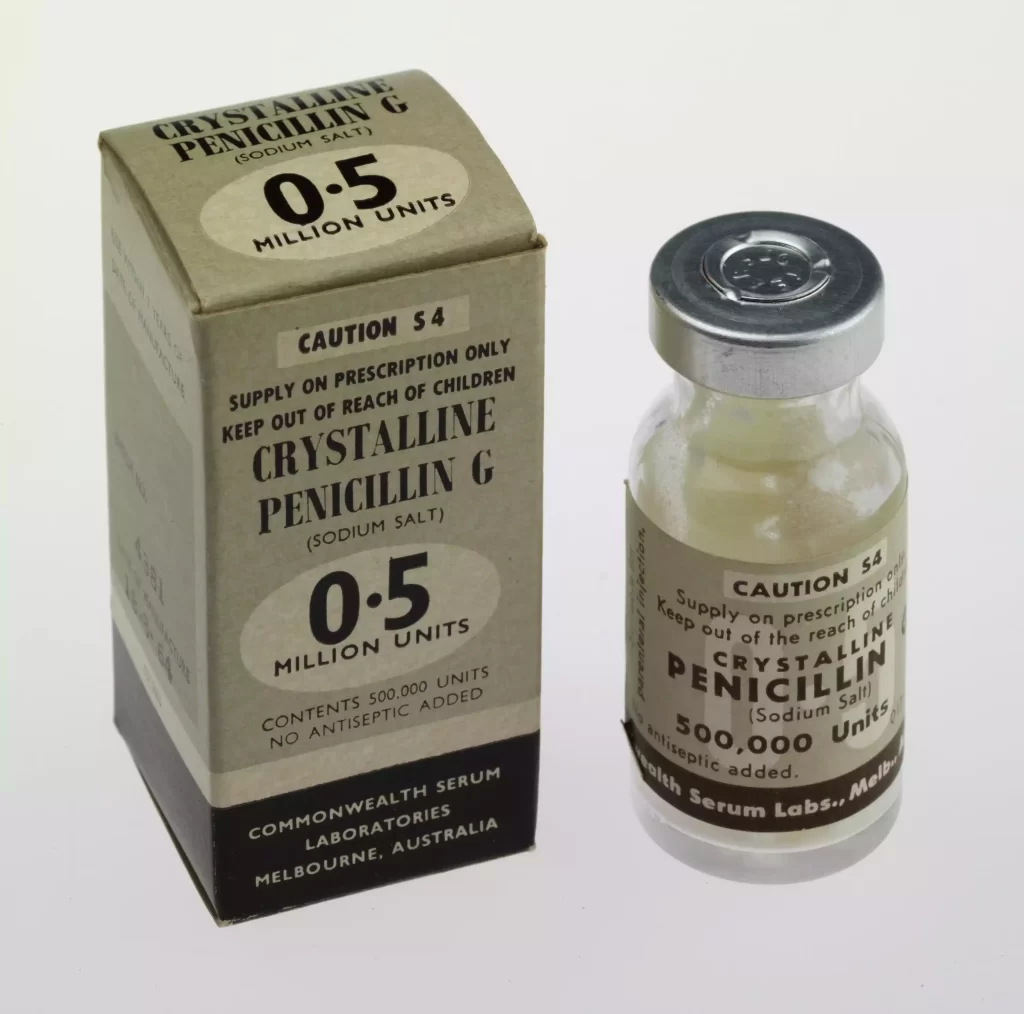
Crystalline Penicillin remains an invaluable medicine, providing effective relief against streptococci, staphylococci, and Gram-negative bacteria infections. Unfortunately, its usage has declined as more stable oral penicillin derivatives such as amoxicillin or ampicillin have come onto the market.
Crystalline Penicillin may not be suitable for all patients as it may lead to allergic reactions; also antibiotic resistance is becoming an increasing threat so its prudent usage must be utilized prudently.
What is Benzylpenicillin?
Benzylpenicillin, commonly referred to as penicillin V, is an antibiotic belonging to the penicillin class that was first discovered by Alexander Fleming. As with other penicillins, Benzylpenicillin shares its beta-lactam ring structure with other penicillins which allows it to effectively fight various bacterial infections. For convenient administration orally and absorption in acidic environments.
Benzylpenicillin antibiotic is widely used to treat less serious infections, including streptococcal throat infections, dental abscesses, and mild skin and respiratory tract infections.
Though less potent against certain bacteria than its penicillin-derivative peers such as amoxicillin or ampicillin (which are more versatile and can be given intravenously), benzylpenicillin remains an invaluable tool when oral therapy is appropriate.
Although benzylpenicillin may cause allergic reactions when taken orally prudent use is necessary in order to combat antibiotic resistance among bacteria populations.
Structure and Formulation
Crystalline Penicillin:
- Structure: Crystalline Penicillin has a structure that is a highly refined type of penicillin that has a clearly defined chemical structure. It is part of the class of antibiotics known as b-lactam. Its basic structure is a b-lactam-like ring that has four members, which is then fused to a thiazolidine ring with five members. Its unique design is the reason for its antimicrobial capabilities.
- Formula: Crystalline Penicillin is produced via a controlled process of fermentation with Penicillium molds. The end product is a white, crystal powder that is high in terms of purity. The purity reduces the possibility of impurities which could trigger adverse reactions. It is easily dissolved in water and can be made for intravenous or oral administration.
Benzylpenicillin (Penicillin V):
- Structure: Benzylpenicillin which is sometimes referred to as Penicillin V, has the same basic b-lactam structure that is found in Crystalline Penicillin. It is, however, the penicillin that is naturally produced and comes directly from the Penicillium mold. Its structure is the foundation for the majority of penicillin antibiotics. This “benzyl” part in its name is a reference to the benzyl group that is attached to the nitrogen atom within the B-lactam rings.
- Formulation: Penicillin V is not as pure compared to Crystalline Penicillin. It comes in many formulations, such as intramuscular solutions and injectable solutions. The composition that is used in the formulation of Penicillin V may vary depending on the manufacturer and may also contain some impurities or other ingredients to increase its stability. Because of its low stability, Penicillin V frequently requires refrigeration to ensure its effectiveness.
Stability and Storage
Crystalline Penicillin:
Stability Crystalline Penicillin is renowned for its durability. Crystalline Penicillin has a long shelf-life in comparison to other types of penicillin. Its stability is the result of the higher level of purification in its production process, which eliminates contamination and impurities that can result in degradation.
Storage: To ensure its efficacy and stability Crystalline Penicillin needs to be stored in a cool, dry place. Below are some specific storage conditions:
- Temperature Storage: Keep between 20degC and 25degC (68degF to 77degF) to get the best results.
- Protection from humidity: Keep the medication away from damp or humid places.
- Protection from sunlight Storage: Store Crystalline Penicillin in containers that protect it from direct sunlight and strong light. This is because exposure to light may cause degrading.
- Make sure that the container is sealed properly: seal the container completely at the end of each use to keep moisture from leaking into.
Benzylpenicillin (Penicillin V):
Stability: Benzylpenicillin commonly referred to as Penicillin V, is less stable than Crystalline Penicillin. It is more susceptible to degradation, particularly after exposure to humidity or extreme temperatures. This lack of stability requires extra care during transport and storage.
Storage: To preserve the stability of the Benzylpenicillin (Penicillin V) and extend its shelf-life The following storage requirements should be adhered to.
- Refrigeration: Keep Penicillin V in a temperature of 2degC and 8°C (36degF between 46 and 36degF) in an air-tight refrigerator. The controlled temperature slows the degradation.
- Protect against moisture: Make sure that the product is not wet since exposure to moisture could result in the degradation that the medication.
- Light protection: Similar to Crystalline Penicillin, Penicillin V must be kept in opaque containers that protect it from exposure to light.
Difference Between Crystalline Penicillin and Benzylpenicillin
Crystalline penicillin is used to treat children with bacterial infections, whereas benzylpenicillin is used to treat adult bacterial infections. So, this is the main distinction between crystalline penicillin as well as benzylpenicillin.
The manifestation of the reaction of Jarisch-Herxheimer reaction occurs when benzylpenicillin is administered but not when the administration of penicillin is crystalline. The appearance of white patches within the mouth occurs as a result of the drug crystal penicillin, but not benzylpenicillin.
Here’s a comparison chart outlining the key differences between Crystalline Penicillin and Benzylpenicillin:
| Aspect | Crystalline Penicillin (Penicillin G) | Benzylpenicillin (Penicillin V) |
|---|---|---|
| Chemical Structure | Highly purified, crystalline | Natural form obtained from molds |
| Formulation | White crystalline powder | Injectable solutions, intramuscular preparations |
| Purity | Highly pure | Less purified, may contain impurities |
| Stability | More stable | Less stable, requires more cool refrigeration |
| Shelf Life | Longer shelf life | Shorter shelf life |
| Route of Administration | Oral, intravenous | Intramuscular, intravenous |
| Medical Applications | Mild to moderate infections | Severe and systemic infections |
| Allergic Reactions | Less likely to cause | More likely, especially due to impurities |
Treatment Efficacy of Penicillin and Benzylpenicillin
The efficacy of treatment is a crucial element in healthcare that evaluates the effectiveness of a treatment in meeting its objectives. In the case of antibiotics, such as Crystalline Penicillin and Benzylpenicillin, knowing the factors that affect the effectiveness of treatment is of vital importance.
Factors Affecting Treatment Efficacy:
- Antibiotic Option: The selection of the most appropriate antibiotic, whether Crystalline Penicillin or Benzylpenicillin, depends on the nature as well as the severity disease. Making the right choice of antibiotic is crucial to the success of treatment.
- Proper Dosage Making sure you are administering the proper dose of antibiotics is vital. Dosing too much could not help in combating the disease, and overdosing could cause negative reactions and can contribute to resistance to antibiotics.
- Absorption by the patient: The patient’s compliance to the treatment plan prescribed by their doctor is crucial. Patients should follow the complete course of antibiotics prescribed by their doctor to ensure that the infection has been completely eliminated.
- Resistance to Antibiotics: The presence of antibiotic-resistant bacteria could significantly affect the effectiveness of treatment. Resistance to antibiotics can render certain antibiotics ineffective which means that alternative treatment options are required.
- Bacterial Susceptibility the susceptibility of bacteria infected with the antibiotic is an important factor in the efficacy of treatment. The antibiotic should be targeted at the specific pathogen that causes the disease.
- Proper timing: Initiating antibiotic treatment promptly is vital, particularly in cases of serious infections. Delaying treatment could cause the infection to get worse and decrease the likelihood of a positive result.
- Quality and purity: The quality and purity of the antibiotic, which includes aspects like a proper storage system and stability, can directly affect the effectiveness of the antibiotic. Incorrectly processed or degraded antibiotics could prove ineffective at treating infections.
- Treatment Combination: Sometimes it is essential to increase the effectiveness of treatment especially in the case of multidrug-resistant bacteria.
Monitoring and Adjusting Treatment
Effective healthcare requires constant evaluation and adjustment of treatment regimens. When administering antibiotics like Crystalline Penicillin and Benzylpenicillin, it’s critical to carefully observe patient response and make adjustments as necessary.
Care providers rely on regular assessments of their patient’s condition from clinical improvement and potential side effects to guidance in making informed decisions. If the patient’s condition does not improve or worsens as expected, adjustments may be required, such as switching antibiotics, altering dosage amounts, or investigating alternative therapies.
By being proactive about making adjustments as necessary to meet individual patient needs and increase chances for successful therapeutic results, adjustments will ensure treatment remains tailored specifically to individual patient requirements and thus increase success rates of therapeutic interventions.
Preventing Treatment Failures
The prevention of failures of treatment in the course of antibiotic therapy is an essential goal of healthcare. There are several strategies that contribute to achieving this goal.
- Affordable Antibiotic Selection: Healthcare providers need to select the correct antibiotic based upon the severity and type of the illness and ensure that it is able to target the pathogen responsible efficiently.
- Correct Dosage: The correct dosage is essential. Dosing too much can not completely eliminate the infection, and excessive dosage can cause adverse consequences and even resistance.
- Patients Adherence: It is imperative that patients adhere to prescribed regimens of treatment in a strict manner to complete the entire course of antibiotics, and to avoid the possibility of relapses or developing resistance.
- Monitor and Adjustment: Monitoring of patients regularly lets healthcare professionals assess the patient’s progress and make changes to their treatment plans.
- Infection Control: The practices of infection control in healthcare settings aid in preventing resistance-producing bacteria from spreading as well as nosocomial infections.
- Antibiotic Stewardship: Implementing programs for antibiotic stewardship assures responsible and judicious usage of antibiotics while minimizing the development of resistance.
- Education and awareness: Education of the patient and the provider about the use of antibiotic resistance, as well as hygiene techniques, are vital to preventing the failure of treatment.
How do Crystalline Penicillin and Benzylpenicillin affect the Environment?
Manufacturing and Discharge:
Processes for manufacturing pharmaceuticals may cause the discharge of Active Pharmaceutical components (Ingredients) (APIs) as well as other chemicals in the environment, which includes water bodies. The discharge could lead to an increase in antibiotics found within water systems of natural origin.
Development of Antibiotic Resistance:
Environmental contamination with antibiotics even at very low levels could contribute to the growth of antibiotic-resistant bacteria in different ecosystems. This can be a significant public health threat since antibiotic resistance could render drugs less effective in treating illnesses.
Ecological Impact:
In the presence of antimicrobials, our environment could disrupt ecosystems that are natural and cause harm to aquatic life, which includes fish and other living things. These chemicals can alter the balance of microorganisms within lakes and rivers.
Human Health Risks:
Antibiotic residues that are present in the environment may get into the food chain resulting in human exposure to very low quantities of the antibiotics. The research is continuing to determine the possible health hazards associated with the exposure.
Wastewater Treatment:
A variety of antibiotics, including Crystalline Penicillin and Benzylpenicillin, aren’t easy to eliminate completely from traditional wastewater treatment facilities, which can lead to their dispersal into the surrounding environment.
Pharmaceutical Waste:
Improper disposal of unused prescriptions or expiring antibiotics by health facilities or pharmaceutical companies could cause contamination of landfills, and even be absorbed into soil.
What is the side effect of Crystalline Penicillin and Benzylpenicillin?
Both Crystalline Penicillin (Penicillin G) and Benzylpenicillin (Penicillin V) are antibiotics belonging to that class known as penicillin. While they can be considered safe, effective, and reliable in treating bacterial infections, they could cause adverse reactions in some people.
Common side effects of crystalline Penicillin and Benzylpenicillin can include:
- Allergic Reactions A very serious possible side consequence of penicillin is reactions to an allergen. It can be minor itching and rashes, and severe reactions which could be life-threatening. The frequency of allergic reactions is higher when Benzylpenicillin is used, particularly for those with an allergy to penicillin.
- Gastrointestinal Disturbances Both antibiotics may cause gastrointestinal adverse effects, such as diarrhea, nausea, vomiting, and abdominal pain.
- Skin Reactions Certain people may have skin reactions, such as itching, rashes, or hives after taking penicillin.
- Oral Thrush In certain instances using these antibiotics may alter the balance of microorganisms within the mouth. This can lead to oral thrush, which is a fungal disease that manifests as white spots in the mouth.
- Yeast infections: Penicillins can also disrupt healthy bacteria balance inside the body, leading the body to develop yeast infections, particularly in the mouth and the genital regions.
- Superinfections Antibiotics, such as penicillins, may disrupt the balance of bacteria within the body. This can cause the growth of fungi and bacteria resistant to treatment which can lead to superinfections.
- Renal Impairment In certain instances penicillins could interfere with kidney function. People with kidney problems that preexist could be more at risk.
- Neurological Signs and Symptoms Rarely, some patients may experience neurological symptoms, such as seizures, confusion or other disorders of the central nervous system.
- Blood disorders: While uncommon, penicillin may affect the number of blood cells, creating conditions such as thrombocytopenia or neutropenia.
Summary
Benzylpenicillin, commonly referred to as penicillin V, is an orally administered antibiotic derived from Alexander Fleming’s original penicillin discovery. Effective against various bacterial infections, especially those of lower severity such as streptococcal throat infections and dental abscesses, such as streptococcal throat infections and dental abscesses.
Its stability in acidic environments enables efficient oral absorption. Though less effective against certain bacteria than its penicillin derivative counterparts, benzylpenicillin still serves as an invaluable treatment option.
As with other penicillins, allergic reactions may arise with its use. Its prudent usage helps combat antibiotic resistance. Benzylpenicillin plays a significant role in healthcare when oral antibiotics cannot treat an infection fully.