Definition of Allergic Rhinitis
Allergic rhinitis, also known as hay fever is a persistent inflammation of nasal passages that is caused through an immune response to certain allergens. If someone suffering from allergic rhinitis breathes in allergens like dust, pollen creatures, dander from animals, or mold the immune system recognizes the substances as harmful and causes the production of histamines as well as other chemical compounds.
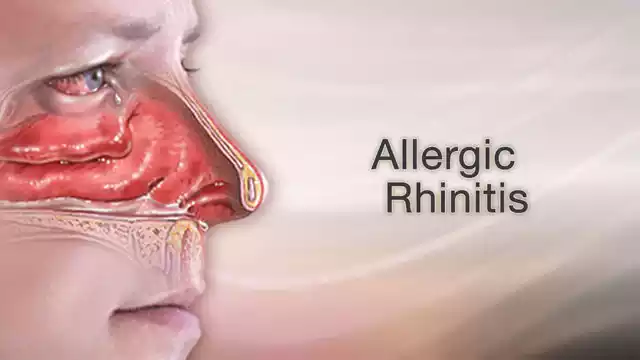
This response to the immune system causes irritation of the nasal passages that results in symptoms such as sneezing itching (in the eyes, nose, or throat) as well as a dry or congested nose, and watery eyes. Allergies can seriously impact the quality of life of a person by creating discomfort that can disrupt sleep and impact daily activities. It could be seasonal, brought on by specific allergens which are present during certain seasons, or chronic, which occurs all year round due to exposure to allergens in the indoor environment.
Treatment options usually comprise allergen-free treatment, medicines such as nasal corticosteroids or antihistamines, and, in extreme instances allergy treatment (allergy shots) to reduce the immune system.
Causes of Allergic Rhinitis
Here are the main causes of allergies:
- Allergens: Exposition to particular allergens causes allergic rhinitis. Common allergens include:
- Pollen: Plants, trees, weeds and flowers let out pollen grains particularly in certain seasons.
- Dust mites: microscopic organisms that are found in dust from the house.
- Animal Dander: Skin flecks that are tiny shed by pets such as rodents, dogs, cats and birds.
- Mold: Fungi that thrive in damp conditions both indoors and out.
- The Immune System Response: For those with allergic tendencies the immune system reacts to harmless substances, interpreting them as a threat. This causes the release of histamines and other chemical substances which cause the appearance of allergic symptoms and inflammation.
- Genetics: Allergy rhinitis is a condition that tends to be passed down through families. People with a allergy history are much more susceptible to develop allergic rhinitis.
- Environmental Factors: Environmental factors such as smoking cigarettes, air pollution and exposure to workplace allergens can cause allergic reactions in people who are susceptible.
- Hygiene Hypothesis: There are theories that suggest improved hygiene and a reduced exposure to certain microbes may increase the incidence of allergic illnesses such as allergic rhinitis.
Symptoms of Allergic Rhinitis
Allergic rhinitis can present a variety of symptoms that typically occur after contact with allergens. This can manifest as:
- Snores: Repetitive and frequent sniffing of the nose, particularly when exposed to allergens.
- Stuffy or Runny Nose: Nasal congestion, with clear discharge or the production of mucus.
- Itching: A sensation that causes itching in the throat, nose eyes, and occasionally in the ear canal or in the roof of the mouth.
- watery eyes: Excessive tearing or eye watering because of the immune response caused by allergens.
- Nasal Itching: Persistent itchiness in the nasal passages that can lead to irritation.
- Postnasal Drip: Mucus drips out from the nasal area to the throat which leads to coughing or irritation.
- Red or watery eyes: Conjunctival redness or irritation caused by allergic inflammation.
- Fatigue: You feel tired, or exhausted due to disturbed sleep caused by symptoms of nighttime like nasal congestion, or postnasal drip.
- A diminished sense of smell and Taste: The temporary impairment or decrease in the ability of smell or taste as a result of nasal congestion.
Definition of Vasomotor Rhinitis
Vasomotor rhinitis is an unallergic condition characterized by persistent nasal symptoms that are similar to those of allergic rhinoitis (such such as runny nose, nasal congestion or postnasal drip) not accompanied by particular allergens or an immune response.

This disorder is caused by the degeneration of nerves and blood vessels inside the nose passages, which leads to symptoms that are triggered by a variety of non-allergic triggers. The triggers could be changes in humidity, temperature or strong odors. They can also be caused by pollution from the air, certain foods and beverages, emotional tension, hormonal fluctuations and other environmental triggers. In contrast to allergic rhinitis, vasomotor rhinitis does not trigger an immune system reaction or the release of histamines.
Patients suffering from vasomotor rhinosis typically have nasal symptoms that remain throughout time, and may experience intermittent exacerbations caused by various external factors. The diagnosis is usually made by determining the cause of allergy through medical history, physical examination and occasionally allergy tests. Treatment options consist of nasal sprays corticosteroids and antihistamines or nasal ipratropium, to ease symptoms, and in some instances, lifestyle changes to prevent triggers.
Causes of Vasomotor Rhinitis
Here are the causes or causes of vasomotor rhinoitis describe:
- Non-allergic factors: Vasomotor rhinitis is most often caused by non-allergic triggers that cause nasal symptoms. A few triggers are:
- Changes in temperature: Abrupt changes in temperature, particularly transitioning from cold to warm conditions or reverse.
- Humidity Variations: Low or high humidity levels can cause irritation to the nasal passages.
- Irritants or Strong Odors: Exposure to strong smells, perfumes, smoke or chemicals, as well as air pollutants can cause irritations to the nose.
- Environmental Factors: Airborne irritants such as dust fumes, pollutants, or even fumes can cause symptoms.
- Certain foods: Spicy foods, hot drinks, or alcohol can trigger nasal irritation for some people.
- The stress of emotional: Stress or emotional causes can cause symptoms to worsen.
- Hormonal Changes: The fluctuation in hormone levels, especially during pregnancy or menstruation, can affect the symptoms of nasal congestion.
- Medical Treatment: Certain medications, particularly blood pressure medication (vasodilators) may be a factor in vasomotor rhinitis occurring in a few cases.
- Nasal Blood vessel Dysfunction: Vasomotor rhinitis can be associated with an abnormal regulation or malfunction of blood vessels and nerves that line these nasal passages. This causes an overactive response to triggers that aren’t allergic, leading to nasal congestion, a runny nose, and postnasal drip.
- Unknown Causes: In many cases the source or trigger of vasomotor rhinitis isn’t immediately identifiable and it is therefore a case of exclusion following the elimination of allergens and other nasal disorders.
Symptoms of Vasomotor Rhinitis
Vasomotor rhinitis is a condition that shares a few signs and symptoms of allergic rhinitis. It is distinguished by a distinct set nasal symptoms that are triggered by non-allergic triggers.
The symptoms could include:
- Nasal Congestion: The sensation of stuffiness, or obstruction in the nose because of swelling nasal passages.
- Runny Nose: Nasal discharge clear, or production of mucus.
- Postnasal Drip: Feeling of mucus flowing into the throat’s back.
- Nasal Itching: The nasal passages can be irritated or itchy.
- Snorting: Sometimes or frequently episodes of sneezing. Usually when triggered.
- Variable symptoms: Symptoms may fluctuate in duration and intensity and are often due to changes in the environment such as stress or non-allergic stimuli.
- Chronicity: Vasomotor Rhinitis symptoms that cause nasal irritation could persist for long periods of time without allergy underlying reason.
- There is no allergen response: Contrary to allergic rhinitis there’s no involvement of the immune system or release of histamines in vasomotor rhinitis.
How to diagnosis of Allergic Rhinitis and Vasomotor Rhinitis?
The process of diagnosing Allergic Rhinitis and Vasomotor Rhinitis is based on a thorough evaluation of the patient’s medical history and symptoms, physical examination and, sometimes certain tests.
Here’s a brief outline of the process for diagnosing to determine the cause of both:
Allergic Rhinitis:
- Medical Histories: The healthcare provider will investigate the patient’s symptoms. This includes the duration of their symptoms of symptoms, seasonal patterns, exposure to allergens of potential and any history of allergies in the family.
- Physical Examining: A nasal examination can identify signs of inflammation like nasal passages that are swollen blue or pale coloration (boggy appearance) and nasal polyps.
- Allergy Testing:
- The Skin Prick test: This involves placing tiny quantities of common allergens on the skin and pricking, or roughing up the skin in order to be able to observe the allergic reaction.
- blood tests (Specific IgE Tests): Blood tests can determine the amount of antibodies (immunoglobulin E or IgE) created in response to specific allergens.
- Response to treatment When symptoms are improved after taking medication for allergies or worsen after exposure to allergens that are known This supports the diagnosis of allergic rhinitis.
Vasomotor Rhinitis:
- Medical Histories: Similar to allergic rhinitis, an extensive background of the symptoms, triggers, as well as their relation to environmental influences is vital.
- Physical Exam: Examination of the nasal passages for indications of inflammation and rule out any other nasal disorders.
- Exclusion of Allergic Causes: Since vasomotor rhinitis can be an exclusion-related diagnosis tests like skin prick tests or IgE tests on blood can be carried out to determine if there are triggers that cause allergic reactions.
- Response for Nasal Medicines, Sprays: Improved symptoms after nasal sprays, such as ipratropium chloride or other prescription medications may help confirm the diagnosis of vasomotor rhinitis.
- Nasal Endoscopy: In some instances healthcare professionals may conduct a nasal endoscopy to check the nasal passages for indications of inflammation.
Treatment and management for Allergic Rhinitis and Vasomotor Rhinitis
Management and treatment strategies for Allergic Rhinitis and Vasomotor Rhinitis seek to relieve symptoms and improve health and quality of life. Here’s a summary of strategies to both disorders:
Allergic Rhinitis:
- Allergen Prevention: Minimize exposure to known allergens such as pollen, animal dander, dust mites or molds. This could include using air purifiers, ensuring that windows are closed when pollen levels are high and cleaning regularly to eliminate dust.
- Medications:
- Antihistamines: The over-the-counter and prescription-based antihistamines can ease symptoms such as itching, sneezing nasal congestion, runny nose, or eyes that are watery.
- Nasal Corticosteroids: They reduce inflammation and can be effective in reducing nose congestion and sneezing and a runny nose.
- Decongestants Decongestants for the nasal or mouth are a short-term relief for nasal congestion, but should only be used for brief time frames due to possible adverse negative effects.
- Montelukast (Leukotriene Modifiers): These may be prescribed to treat allergies to rhinitis. This is especially true in the case of asthma that is concomitantly present.
- Immunotherapy (Allergy Shots or Sublingual Tablets): For individuals who suffer from severe or uncontrolled manifestations, an allergen-based immunotherapy might be suggested. It involves slowly exposing the patient to small doses of allergens in order to de-sensitize to the body’s immune.
- Nasal Rinses: The use of saline in nasal irrigation can reduce nasal congestion as well as remove irritating substances from the nasal passages.
Vasomotor Rhinitis:
- Find and avoid triggers: Patients are advised to identify and limit exposure to triggers that are not allergic like strong odors, smoking, temperature fluctuations or stress.
- Nasal Sprays or Medications:
- Nasal Anticholinergics (e.g. Ipratropium, for example): These sprays can reduce nasal secretions and ease symptoms of vasomotor rhinitis.
- Nasal Corticosteroids: They may also be prescribed to treat inflammation and signs.
- Nasal Saline irrigation: A regular intake of nasal sprays containing saline or rinses can aid in moisturizing nasal passages and ease symptoms.
- Avoid excessive use of decongestants: Limit the use of nasal sprays that decongest the nose, because they could cause chronic congestion if they are used too often.
- Stress management: Stress reduction techniques or counseling could help to combat symptoms that are aggravated by stress.
General Considerations for Both Conditions:
- Talk to a specialist: Consider seeing an allergist or ear, nose and throat (ENT) specialist to conduct a thorough assessment and a customized treatment program.
- Regular follow-ups: Keep in touch with medical professionals to assess symptoms and modify treatment if required.
- Education and Empowerment of Patients: Educate patients about their medical condition, triggers, as well as the significance of adhering to treatment regimens.
Comparison table of Allergic Rhinitis and Vasomotor Rhinitis
Here’s a table that compares the main distinctions in Allergic Rhinitis and Vasomotor Rhinitis:
| Characteristic | Allergic Rhinitis | Vasomotor Rhinitis |
|---|---|---|
| Underlying Cause | Immune system response to certain allergens | Dysfunction of blood vessels as well as nerves that run through the nose. |
| Triggers | Allergens, such as pollen dust mites as well as animal Dander | Non-allergic factors: temperature, odors, stress, etc. |
| Onset of Symptoms | The allergens are triggered immediately upon exposure. | The trigger is caused by non-allergic stimuli. often delayed |
| Duration of Symptoms | Perennial or seasonal, based on the exposure to allergens | Persistent, chronic, or infrequent |
| Symptoms | Itching, sneezing or watery eyes, stuffy nose | Akin to allergic rhinitis however, without specific allergen triggers |
| Immune Response | It involves the immune system and release of histamines. | No involvement of the immune system, or release of histamine |
| Diagnosis | Allergy testing (skin testing with a needle, IgE blood tests) | Diagnostics of exclusion Eliminating allergies as the cause |
| Treatment | Antihistamines, avoidance of allergens and nasal corticosteroids. Immunotherapy | The prevention of triggers and nasal anticholinergics corticosteroids and nasal saline stress management |
This table provides the most fundamental distinctions in Allergic Rhinitis and Vasomotor Rhinitis by highlighting their distinct causes and triggers, immune responses as well as diagnostic strategies and treatments.
Similarities Between Allergic Rhinitis and Vasomotor Rhinitis
Even though Allergic Rhinitis and Vasomotor Rhinitis differ in their reasons and causes, the two have some commonalities:
- Nasal symptoms: Both conditions present with the same nasal symptoms, like nasal congestion, a runny or nasal congestion and postnasal drip, nasal itching, and sometimes sniffing.
- Effect on quality of life: Both of these conditions can greatly affect a person’s quality of life which can cause discomfort, fatigue, sleep disturbances and impacting daily activities.
- Chronicity: both Allergic Rhinitis as well as Vasomotor Rhinitis are chronic diseases with symptoms that continue for a long time. While allergic rhinitis could exhibit seasonal or continuous patterns that are based on exposure to allergens and vasomotor rhinitis may be chronic or intermittent.
- Methods of Management: Management and treatment strategies to treat both diseases can include an application of sprays for nasal use (corticosteroids and anticholinergics) and the use of saline nasal rinses and, in certain instances lifestyle changes to lessen symptoms.
- Diagnosis through Symptoms: The diagnosis for both of these conditions requires a review of the patient’s symptoms as well as health history and physical exam and, in certain instances, excluding other nasal disorders. Both of them may require the exclusion of other underlying causes in order to determine the correct diagnosis.
Although they have a lot in common with the presentation of symptoms and treatment methods The main difference is in the root cause: allergic rhinitis triggers an immune reaction to certain allergens, while vasomotor rhinitis is identified by nasal symptoms that are caused by non-allergic triggers and doesn’t trigger the immune system in a response.
Prevention Strategies
Strategies for prevention of Allergic Rhinitis and Vasomotor Rhinitis are focused on minimizing exposure to triggers as well as managing the root causes of symptoms. Below are a few preventive steps for both ailments:
Allergic Rhinitis:
- Allergen Avoidance:
- Identify specific allergens causing symptoms (e.g., pollen, dust mites, pet dander).
- Make use of air purifiers equipped with HEPA filters to help reduce the amount of allergens in your home.
- Close the windows during peak pollen levels.
- Cleanse bedding frequently with hot water to eliminate dust mites.
- Limit Exposure to Outdoor Allergens:
- Be sure to look up forecasts for pollen counts and make sure you stay indoors in the peak pollen count.
- Change clothes and shower after being outdoors to get rid of pollen.
- Indoor Environment:
- Clean your home and clean frequently.
- Covers that are anti-allergen can be used on mattresses and pillows.
- Take into consideration removing carpets and using a HEPA filtering vacuum.
- Medications:
- Utilize prescribed antihistamines and nasal corticosteroids according to the directions during the allergy season.
- Immunotherapy:
- Allergy shots and sublingual immunotherapy under medical supervision could aid in reducing the immune system’s sensitivity.
Vasomotor Rhinitis:
- Identify and Avoid Triggers:
- Avoid the exposure to triggers that are not allergic, such as intense odors or temperature variations smoking, stress or smoke.
- Environmental Control:
- Keep indoor temperatures stable and levels of humidity.
- Make use of air filtration systems in order to minimize indoor irritations or allergens.
- Nasal Irrigation:
- Make sure to regularly use the nasal sprays and rinses containing saline to keep the nasal passages hydrated and free of irritations.
- Stress Management:
- Try stress-reducing techniques like yoga, meditation or exercising, as stress can cause symptoms to worsen.
- Avoid Overuse of Medications:
- Reduce the use of nasal decongestant sprays in order to avoid rebound congestion.
General Preventive Strategies:
- Consultation with specialists: Seek guidance from allergists and ENT specialists for specific preventive strategies as well as treatment strategies.
- Monitor regularly: Examine the amount of pollen or any environmental variables to avoid potential exposure to triggers.
- Information and awareness: Learn more about the triggers, condition and the appropriate methods of management.
Be aware that individual triggers and reactions are different for each person therefore understanding the specific triggers and seeking guidance from a professional is essential to develop appropriate preventive strategies specifically tailored to the needs of each individual.
Impact on Daily Life
The two Allergic Rhinitis and Vasomotor Rhinitis could significantly affect a person’s everyday life because of the constant and annoying symptoms.
Impact of Allergic Rhinitis:
- Trouble with breathing: Symptoms like nasal congestion, sneezing and itching, and a runny nose can make you feel uncomfortable all day long, making it difficult to concentrate and do tasks with ease.
- Sleep Disorders: Nasal congestion and postnasal drip may disrupt sleep, causing fatigue and a lower level of alertness during the day.
- Lower Productivity: Constant sneezing, watery eyes, nasal congestion can reduce the productivity of students or at work.
- Social and emotional impact: Allergic rhinitis symptoms affect social interactions as well as emotional wellbeing due to continuous irritation and tiredness.
- Interfering with activities: It is possible that symptoms hinder sporting activities, outdoor activities or other activities, particularly during the high pollen seasons.
Impact of Vasomotor Rhinitis:
- Persistent Symptoms: Nasal symptoms such as nasal congestion, a runny nose and postnasal drip could last in a way that causes discomfort and irritation during the entire day.
- Triggered Symptoms: Sensitivity to different triggers that are not allergic can result in sudden or unexpected symptoms exacerbations which can disrupt the planned activities.
- Qualities of life: Like vasomotor rhinitis, allergic symptoms of rhinitis can impact your quality of living, interactions with others and even emotional wellbeing due to constant discomfort.
- Sleep disturbances: Nasal symptoms might affect sleep, causing tiredness and lower energy levels throughout the day.
Coping Strategies:
- Medication Adherence: The proper use of prescribed medications according to the healthcare professional’s guidelines can help treat the symptoms efficiently.
- Strategies to Avoid: Identifying triggers and trying to avoid exposure as much feasible can help reduce symptoms severity and frequency.
- Consultation with healthcare providers: Seeking guidance from health professionals can result in customized treatment plans that meet your individual requirements.
Both diseases require a proper treatment to reduce symptoms and limit their impact on everyday life. Getting medical advice, following prescribed treatments, and making changes to your lifestyle are crucial actions to manage conditions and helping improve overall wellbeing.
Final Opinion
The Allergic Rhinitis or Vasomotor Rhinitis can be described as chronic nose disorders which have similar symptoms, but with distinct causes. Allergic Rhinitis causes an immune response to specific allergens which causes nasal inflammation as well as symptoms like sneezing irritation, as well as a dry or congestion-filled nose. Vasomotor Rhinitis, on the contrary, is triggered by triggers that are not allergic, and can cause nasal symptoms with no the involvement of the immune system.
Although allergic rhinitis is defined by specific allergen responses and vasomotor rhinitis can be characterized by nasal symptoms that are caused by a variety of factors, including variations in temperature, intense smells, or stress. Effective treatment for both of these conditions requires finding triggers, using treatments, lifestyle adjustments and finding individualized treatment plans to ease symptoms and enhance the quality of life for the affected people.

